posted 24th August 2022
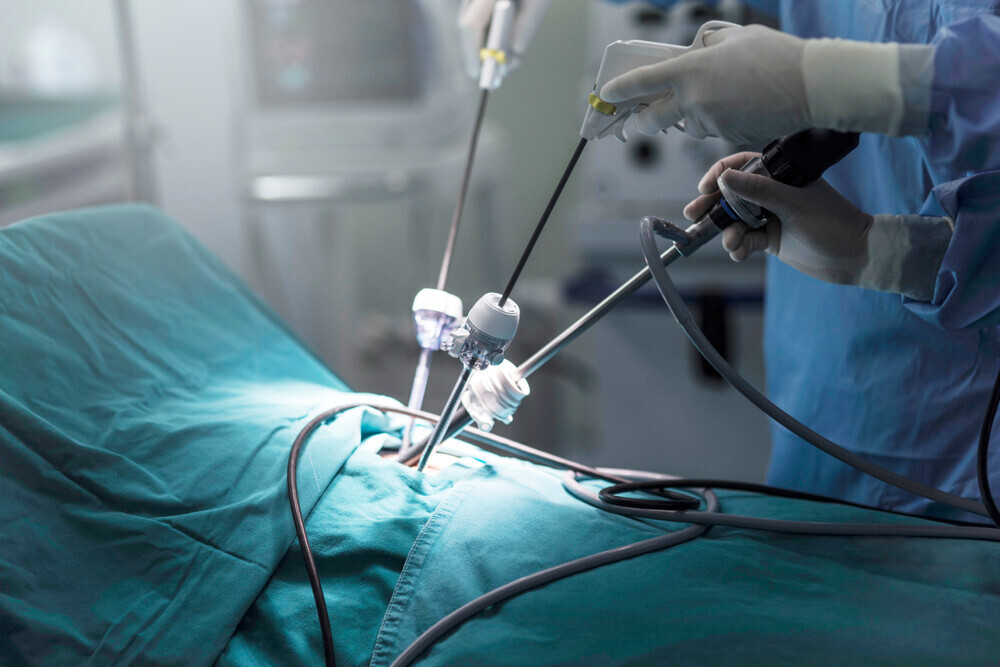
Laparoscopic excisional surgery for severe Endometriosis
Surgery for severe endometriosis can be complex and may require input from other specialities such as colorectal surgery or urology. In most instances, you will have the opportunity to meet with all the relevant specialists involved in your surgery.
Types of surgery:
Two types of surgery are offered. Your doctor will discuss the type of surgery that is appropriate for you.
1: Laparoscopy (keyhole surgery) – this is the most common operation that we offer in our unit.
2: Laparotomy or open surgery – which involves a cut in the abdomen, usually along the bikini line, but in some cases, it may be an “up and down” cut. This depends on the complexity of the case.
What is the aim of surgery?
The purpose of surgery is to make your symptoms better and/or to improve your chances of pregnancy.
How successful is the surgery?
In the vast majority of patients, pain symptoms improved significantly, and they remained well when followed up for 2 years after surgery. Surgery also showed improvement in pregnancy rates. Unfortunately, some patients will develop recurrence of symptoms after the operation, and this is seen in roughly 5-25% of patients when followed up for 2 years.
What does this surgery involve?
Surgery for severe endometriosis involves cutting away endometriosis from affected areas and freeing up of organs (adhesiolysis). In severe disease, there might be involvement of important organs in the pelvis like the bowel, bladder, ureter and pelvic nerves. Surgery to remove endometriosis involves operating on or near these structures.
Below is a description of some of the procedures. It is important to understand that more than one organ may be involved, and a combination of procedures may be required. Specific procedures may be required for endometriosis affecting the bowel, bladder and ureters.
Endometriosis involving the bowel:
This may involve any of the following procedures
- Adhesiolysis – this involves freeing of the bowel from endometriosis
- Shaving – includes cutting out the lesion from the surface of the bowel without entering the lumen (opening) of the bowel.
- Disc resection – involves using a circular stapler to cut away a small circular piece of the bowel.
- Anterior resection – a segment of the bowel is removed, and the healthy ends are joined together using staples.
Endometriosis involving the bladder:
Endometriosis involving the bladder may require a part of the bladder to be excised (partial cystectomy). Most of the lesions can be cut away without breaching the cavity if the lesion has not gone too deep into the bladder. The bladder usually heals very well, but you are likely to need a catheter for 7-14 days.
Endometriosis involving the ureters:
Ureters are the tubes that carry urine from the kidneys to the bladder. Most of us have two ureters – one on each side. If endometriosis involves the ureters, it can cause compression and damage to the kidneys. The majority of lesions involving the ureters are due to compression caused by endometriosis in the surrounding tissues. Such obstruction can be relieved by freeing the ureter (ureterolysis) and excising the lesion from the surrounding areas. In some cases, a stent may be inserted to protect the ureters during surgery to allow healing of a traumatised ureter. This may be removed either at the end of surgery or after 4- 6 weeks.
If the compression or stricture of the ureter cannot be relieved by ureterolysis (freeing the ureter from a lesion of endometriosis), this part of the ureter may be excised, and the healthy ends are either joined together or where this is not possible, a new connection is made into the bladder (re-implantation). This is very rarely required. Most ureteric lesions can be treated laparoscopically (keyhole), but in some cases, open surgery may be required.
Risk and complication of surgery for severe endometriosis:
General risks:
- Risk related to the anaesthesia.
- Bleeding.
- Infection
- Blood Clots in legs and lungs (DVT and PE)
- Conversion of laparoscopy to an open procedure either due to the severity of disease or to deal with a complication
- Late complications like infection, bleeding, haematoma (blood clot), port-site hernias
Specific risks relating to different organs
Bowel
Complications involved in bowel surgery may be either during the operation (intraoperative) or late (after the operation). The most common intraoperative complication is unintended: perforation of the bowel (chance is less than 1in 100). In most patients, the perforation can be repaired without any consequences. This is why we give “bowel prep” to patients undergoing such surgery so that such repairs can be carried out. In some patients, a stoma may be needed to allow the repaired part of the bowel to heal. A stoma is an opening in the stomach connecting the bowel to the outside to divert stools from going through the repaired part of the bowel, thus allowing it to heal in the meantime. The stool will be collected in a sealed bag attached to the opening in your tummy. This is usually a temporary measure and is reversed after a few weeks/months. In some cases, surgery may sometimes be converted to an open procedure (up and down or across cut in the tummy).
Late complications following bowel surgery include:
- perforation, anastomotic leakages (leaking of faeces from newly joined segments of bowel after anterior or disc resection),
- abscesses and rarely rectovaginal fistulas (the connection between bowel and vagina – with faeces leaking through the vagina). These are rare and occur roughly in about 3 out of 100
- bowel operations.
Anterior resection syndrome
This is a combination of different symptoms experienced by patients undergoing anterior resection. Symptoms include constipation, increased frequency of stools, urgency, incontinence to flatus (gas) or faeces, incomplete emptying and passing of small stools (fragmentation). Increased frequency and incontinence to flatus have been the main symptoms noted in endometriosis patients after bowel resection.
Bladder and ureter
If you had a partial excision of the bladder wall (partial cystectomy), a urinary catheter might be left in place for 7-14 days. We will always check if the bladder has healed by doing an x-ray (cystogram). In rare instances where the healing has not taken place, the catheter may be left longer, or you may be offered further surgery. If you have a stent in place, this is usually removed after a few weeks. This might cause pain and infection.
Risks with ureteric surgery include:
Non-healing of the ureter leading to leakage of urine into the tummy causing pain and ureteric fistula (urine leaks into the vagina). These are very rare and will usually require further surgeries (laparoscopic or open).
Other late complications include haematoma (blood clots), difficulty in voiding (very rarely patients may experience long term problems with voiding after deep excision of endometriosis due to damage to pelvic nerves).
Perioperative Complications
(During Surgery) – 5%
Excessive bleeding – <10 in 1000
Unexpected bladder injury -<10 in 1000
Unexpected ureteric injury -<10 in 1000
Unexpected bowel injury -10 in 1000
Risk of Stoma – 1 in 200
Post-operative complications
Haematoma -<10 in 1000
Pelvic abscess -<6 in 100
Urinary leak – <8 in 1000
Bowel leak – <10 in 1000
Fistula – <4 in 100



